News
Posts Tagged ‘dogs’
Management of Atopic Dermatitis in Dogs and Cats
by admin on June 1st, 2016
Category: News, Tags: Tags: atopic dermatits, cats, dogs, pets
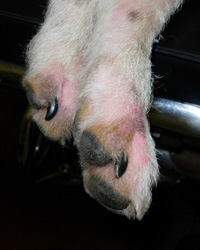
Last month we explained what atopic dermatitis is and how it is diagnosed. In this article we consider how atopic dermatitis can be managed in affected dogs and cats.
Can I cure atopic dermatitis?
In one word “No”, but you can manage the condition successfully. Atopic dermatitis in dogs and cats can be compared to asthma in people. Asthma can’t be cured but it can be managed; and just like asthma the management of atopic dermatitis is life-long. It is therefore important to put in place measures that are going to have the least side-effects for your pet in the long term that will provide him/her a good quality of life and that are the most cost effective and affordable for you.
How can I manage the condition?
You need to take a multi-step approach to managing atopic dermatitis. These steps include:
- Treatment and prevention of infections
- Medications to stop the itch
- Treatment that modulates the immune system
- Nutritional supplements
- Topical treatments
- Unfortunately some treatments work some of the time but not all the time and so you may need to switch treatments periodically. Some treatments may result in undesirable side effects and so may need modification.
Management options:
1) Treatment and prevention of infections:
Any bacterial (mostly staphylococcal) and/or yeast (Malassezia) infections should be treated at the outset. Antibiotics for bacterial infections need to be administered for 7 – 14 days beyond clinical cure and the duration of treatment is generally determined by the depth of the pyoderma.
For yeast infections a shampoo containing either 2% chlorhexidine/2% miconazole or one containing 3% chlorhexidine have shown good efficacy and will suffice; however, if the infection is severe your vet may opt to prescribe antifungal tablets. Because there is a tendency for infections to recur it is best to bath your pet once or twice a week on a regular basis, which will keep the microbial load on the skin low and thus help reduce the frequency of infections.
2) Stopping the itch:
Glucocorticoids (steroids) will stop the itch in most cases, but need to be used with caution, especially if used for a long time. In the short term they can increase water intake, increase urination and appetite. Some owners and pets find these side effects distressing. In the long term they can affect almost any organ in the body, therefore, even when well tolerated, they should be used with caution and your pet should be monitored regularly. Topical steroid containing sprays and ointments may be useful for targeted areas but with long term use thinning of the skin, infections and systemic side effects can occur.
Cyclosporin is used to damp-down (modulate) an over-reacting immune system in an atopic pet. One starts with a high dose and then tapers it down to alternate day, or better still twice a week, treatment. The most common side effects with ciclosporin are vomiting and diarrhoea. In some dogs, gingival hyperplasia and papillomas may also occur.
Oclacitinib is another immunomodulating drug which specifically targets the pathway that results in an itch. It is effective and can stop itching rapidly. This is the newest drug on the market and the reported side effects are vomiting and diarrhoea in a small number of cases. It can be used both short term and long term; however, given that this drug has now been on the open market for only a few months (at the time of writing this) it should be used with caution as side effects with prolonged use are not known.
Antihistamines; the response to this group is variable and they are often used in combination with steroids in order to reduce the steroid dose.
3) Immune Modulation:
Allergen specific immunotherapy is the most specific treatment for Atopic Dermatitis. It involves either an injection, or an oral dose of the allergens your pet is allergic to, to modulate the immune system. It has responses ranging from roughly 33% where there is complete cessation of itch, to 33% improving but requiring additional treatments, to 33% where there is no response. If your pet responds well to immunotherapy, it is likely to have the least adverse side-effects and to be the most cost effective treatment in the long term.
4) Nutritional support:
Omega -3 and Omega -6 essential fatty acids help the skin function by altering the lipid barrier and by reducing inflammation. On their own they are unlikely to benefit your pet but can be helpful when combined with other treatments. Diets that are high in essential fatty acids (EFAs) also help.
5) Topical treatments:
Moisturisers containing ceramides help maintain the skin barrier, which in turn reduces the penetration of allergens and therefore your pet’s reaction to them. Bathing with an oatmeal based shampoo can also help relieve itching and re-hydrate the skin.
Atopic dermatitis is a lifelong condition that requires life-long management; and often more than one type of treatment will be required. So, when your vet chooses a treatment, it should be efficacious, suitable for your pet with the least side effects, easy for you to administer and affordable. Most of all it/they should improve your pet’s (and your) quality of life.
CRUCIATE DISEASE IN DOGS
by admin on April 1st, 2016
Category: News, Tags: Tags: cruciate disease, dogs, highland terrier, labrador, mastiff, rottweiler

Injury or failure of the cranial cruciate ligament (commonly referred to as Cruciate Disease) is a very common problem that can be encountered by dogs of all shapes and sizes. Some breeds such as the Labrador Retriever, Rottweiler, Mastiff breeds and West Highland white terrier appear predisposed whereas some breeds such as greyhounds are seldom affected. Cruciate disease is the most common reason for orthopaedic surgery being performed and the most common reason for referral to a specialist orthopaedic surgeon being considered. Cruciate ligament rupture also occurs in cats but is far less common.
What are the cruciate ligaments?
Ligaments are tough bands of tissue situated in and around joints to provide stability whilst still permitting normal movement of the joint. There are two cruciate ligaments found within the stifle (knee) joint – the cranial cruciate ligament and the caudal cruciate ligament. The cranial cruciate ligament originates between the condyles (knuckles) of the femur and passes diagonally forwards and medially (towards the inside of the joint) to attach on the upper surface of the tibia. The caudal cruciate ligament sits behind the cranial cruciate ligament and passes in the opposite diagonal (from medial to lateral). When both cruciate ligaments are viewed from the front of the joint they form a cross or X shape, hence the name cruciate.
The cranial cruciate ligament is more important than the caudal cruciate ligament and is responsible for preventing three movements that may become apparent where the ligament fails:
- Tibial thrust – The tibia slides forwards in relation to the femur, leading to the sensation that the joint will not lock out when standing/walking.
- Internal tibial rotation –the tibia and lower limb pivot around the long axis of the bone. This may result is the paw turning inwards when the foot touches the floor, a so called pivot shift.
- Hyperextension – Some dogs will cause rupture the cruciate ligament by hyperextending the stifle joint. This most commonly happens where the hindlimb gets caught in a fence whilst jumping.
Why do cruciate ligaments become injured?
The majority of dogs develop rupture of the cruciate ligament as a consequence of a degenerative process where the fibres within the ligament gradually break down. The cause of this degeneration is unproven at this time. Ligament degeneration occurs with normal activity and can take many months. Owners frequently report intermittent periods of mild lameness that then seem to resolve spontaneously. Unfortunately the ligament is typically getting progressively weaker and eventually will rupture. Some dogs can be persistently lame with a partial tear of the cruciate ligament, where others will only become lame at the point of complete rupture.
A relatively small proportion of dogs will injure their cruciate ligament during a traumatic incident, such as where the limb is caught in a fence. If cruciate rupture has resulted from such an accident, there will often be other damaged ligaments that must be recognised and appropriately treated if limb function is to be restored.
How can you be sure that the cruciate ligament has failed?
The diagnosis of cruciate disease can be made based on clinical examination in the majority of cases. There is typically a hindlimb lameness that varies from mild to non-weight bearing. The affected stifle joint is often painful and distended with fluid. A pad of fibrous tissue called a medial buttress may develop on the medial side of the tibia in longstanding cases. The most important tests for cruciate rupture are the cranial drawer and tibial compression tests. These are performed by your veterinary surgeon and are tests of joint stability that aim to detect the tibia sliding forwards in relation to the femur. An abnormal degree of this movement indicates rupture of the cranial cruciate ligament. With recent complete ruptures, the instability is generally very obvious, however where there is a partial tear or a very longstanding cruciate rupture, the degree of instability can be virtually undetectable. Where this occurs assessment of the joint by MRI or by direct surgical assessment may be necessary to confirm the diagnosis.
What happens to the joint after a cruciate rupture?
Cruciate injury causes the release of pro-inflammatory substances within the joint. This inflammatory response causes a cycle of events that results in the inevitable and irreversible degeneration of articular cartilage that we know as osteoarthritis. As cartilage degenerates it becomes more fragile and susceptible to injury as a result of the abnormal shearing forces exerted on the now unstable joint.
The joint surfaces of the femur and tibia are separated by two fibrocartilage pads, each called a meniscus. Each meniscus is shaped like a flattened kidney bean and is fixed within the joint by other small ligaments. When considered as a unit, the two menisci form a shallow dish of fibrocartilage that act as a shock absorber to reduce the pressure exerted on the underlying cartilage. Following cruciate rupture, the medial meniscus frequently becomes damaged as a result of being crushed between the joint surfaces as the tibia shifts forwards underneath the femoral condyle. The damaged meniscus is painful and can become trapped between the joint surfaces, causing further damage to the joint surface. The recognition and treatment of meniscal injury is an important part of the surgical management of cruciate disease.
It is an unfortunate reality that degenerative cruciate disease often occurs simultaneously in both stifle joints. Approximately 60% of dogs sustain a cruciate rupture in the other stifle joint within 18 months of the first side failing. Occasionally we see dogs where both cruciate ligaments have ruptured simultaneously. This causes substantial problems walking as both hindlimbs are painful and it is not uncommon for the symptoms to be mistakenly attributed to a spinal cord injury.
Will my pet always be lame after a cruciate rupture has occurred?
It is possible to successfully manage almost all cases of cruciate rupture successfully. The best outcomes are most consistently found following surgical intervention to improve joint stability and treat meniscal injury. Some dogs will regain reasonable function without surgery, however in general most conservatively managed dogs will be persistently lame with varying degrees of muscle wastage, restricted range of motion and ongoing joint pain.
There are a multitude of surgical treatment options that may be applied to dogs and cats with cruciate disease. Part 2 of this article will discuss the various treatment options that are available.

