News
Inflammatory Bowel Disease (IBD)
by admin on June 6th, 2019
Category: News, Tags:
What is IBD?
IBD is a disease that causes inflammation in any part of the digestive tract (stomach and/or intestines and/or colon i.e. large bowel). Some breeds of dog, such as Soft Coated Wheaten Terriers have a genetic predisposition to this disease. In other breeds of dogs and cats it can be triggered by a parasite or food intolerance. More commonly no specific underlying cause is found and the disease is thought to be caused by an over-activity of the body’s immune system (which normally fights off infections) to ‘foreign’ proteins (such as food) that are eaten, resulting in inflammation.
What are the signs of IBD?
- Weight loss
- Vomiting
- Diarrhoea
- Increased or decreased appetite
- Blood or mucus in the faeces
How is IBD diagnosed?
IBD is diagnosed by a combination of tests, as several other diseases can cause similar signs. Blood tests are often performed to rule out other underlying diseases such as liver or kidney disease, and faecal examination is performed to look for any parasites. Cats with IBD can have low vitamin B12 levels therefore vitamin B12 is measured in all cats.
As foreign body obstructions, or sometimes tumours, can cause weight loss and vomiting, X-rays or ultrasound scans are usually performed to rule out these problems.
Finally, the ultimate diagnosis of IBD is made by taking biopsies from the stomach, intestine or colon. Usually this is performed under a general anaesthetic using a flexible endoscope camera, of which we have several different sizes to suit different sizes of patient. This is not an invasive procedure and most pets recover very quickly and will go home within 24 hours.
How is IBD treated?
Many dogs and cats will improve following a dietary trial. Often this involves prescribing a new diet that is hypoallergenic (i.e. unlikely to cause a reaction) or contains a protein source that your pet has not eaten before (such as venison or salmon). This is fed for 1 to 2 months and it is very important that no other food, treats or tit-bits are given. Some pets won’t respond to one diet but will respond to an alternative diet.
Pets that don’t respond to diet alone may be prescribed certain antibiotics.
Dogs and cats that are severely affected or that don’t respond to the treatments mentioned above will be prescribed steroids. A high dose is prescribed initially and this is decreased every few weeks for several months. Sometimes in pets that don’t tolerate steroids or don’t respond to steroids alone, other drugs which suppress the immune system are prescribed.
What is the long term outlook? (prognosis)?
IBD has a broad spectrum of severity, ranging from mild vomiting and diarrhoea to severe weight loss and fluid build up in the abdomen. It is not generally a life-threatening disease but can be in severely affected patients. It is not a curable disease, therefore the aim of treatment is to minimise the frequency of vomiting and diarrhoea: it is rare to be able to stop the clinical signs altogether. Keeping a diary of how often the signs are happening can be helpful to us in establishing the success of treatment. Most dogs and cats are able to live a good quality of life following a diagnosis of IBD.
Pet of the month – June 2019
by admin on June 6th, 2019
Category: Pet of the Month, Tags:
IBD is not a single disease but a group of chronic gastrointestinal disorders caused by an infiltration of inflammatory cells into the walls of a cat’s gastrointestinal tract. The infiltration of cells thickens the wall of the gastrointestinal tract and disrupts the intestine’s ability to function properly.
IBD occurs most often in middle-aged and older cats.
How is IBD diagnosed?
Symptoms of feline IBD are not specific. They may include vomiting, weight loss, diarrhea, lethargy and variable appetite.
The symptoms of IBD can vary depending on the area of the digestive tract affected.
A definitive diagnosis of feline IBD can only be made based on microscopical evaluation of tissue collected by means of an intestinal (or gastric) biopsy.
How is IBD treated?
The treatment of IBD usually involves a combination of change in diet and the use of various medications. There is no single best treatment for IBD in cats. Your veterinarian may need to try several different combinations to determine the best therapy for your cat.
Hypoallergenic diets are usually tried first. Corticosteroids like prednisolone may be used to reduce inflammation of the gut, and antiobiotics such as metronidazole are commonly used.
What does the future hold for a cat with IBD?
IBD is a chronic disease. Few cats are actually cured. Symptoms of IBD may wax and wane over time. IBD can often be controlled such that affected cats are healthy and comfortable. Vigilant monitoring by the veterinarian and owner is critical.
We are very pleased to report that Bob has responded well to dietary management and is currently not requiring additional medication. Luckily he is not adept at hunting and so we have no fear that he might upset the illness through illicit snacks!
Arthrodesis
by admin on April 30th, 2019
Category: News, Tags:
What is arthrodesis?
Arthrodesis means the surgical fusion of a joint. In other words, the bones forming the joint are permanently joined together so that there is no movement in this part of the limb. Arthrodesis is a salvage procedure that is generally only performed when there are no other options to save the function of the joint.
What joints can be arthrodesed (fused)?
The shoulder, elbow, carpal (wrist), stifle (knee), hock (ankle) and digit (toe) joints can be arthrodesed. The main joint that cannot be fused is the hip joint. This is generally not a problem since the hip joint can be replaced with an artificial one. Elbow and knee replacements are also possible alternatives to arthrodesis of these joints.
Reasons for performing an arthrodesis
The principle indications for arthrodesis are:
- osteoarthritis that is causing chronic pain and cannot be managed medically
- joint instability that cannot be treated by other means
- fractures involving the joint surface that cannot be repaired
- infection involving the joint that fails to respond to antibiotics
- tumours in or around joints
- muscle/tendon rupture that cannot be managed directly
What does arthrodesis involve?
There are a number of important steps when fusing a joint:
- the surface of the joint (known as the articular cartilage) must be removed to enable bony fusion.
- a bone graft should be placed into the spaces between the bones to promote fusion. This may be an autograft (from the patient), an allograft (from a donor) or a combination of both.
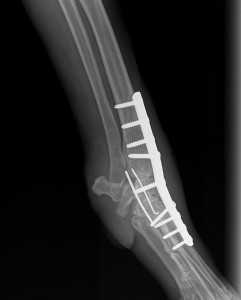
- the bones forming the joint to be arthrodesed must be rigidly stabilised to maximise the possibility of bony fusion. This is most commonly achieved with one or two plates that are secured to the bones under the skin. Occasionally an external skeletal fixator (a metal framework) is employed, where the bones are stabilised with pins that penetrate the skin and are attached to bars on the outside of the limb.
- exercise must be restricted until there is radiographic (X-ray) evidence that the bones have fused. This often takes eight to 12 weeks.
Risks and complications
The majority of arthrodesis operations are uneventful and are not associated with complications, however, these are major procedures and thus the following complications are possible:
- loosening or breakage of implants (plates, screws, pins) may occur if the joint fails to fuse in sufficient time. Implant failure can result in joint instability and necessitate further surgery.
- wound problems, such as breakdown and infection, are primarily associated with arthrodesis of the carpal (wrist) and hock (ankle) joints. Wound management within the first few weeks of surgery is of vital importance to minimise this risk. Dressings are often applied to the limb to minimise swelling and prevent the patient interfering with the wound.
- fracture of bones adjacent to the fused joint may occur due to the abnormal forces that result following arthrodesis surgery.
How good is limb function following arthrodesis surgery?
Limb function after arthrodesis surgery is primarily dependent on which joint is fused. It is good following carpal (wrist) and hock (ankle) arthrodesis and fair following shoulder arthrodesis. Fusion of the elbow or stifle (knee) joint significantly compromises limb function. Dogs and cats generally have to swing the limb outwardly (circumduct) when walking in order to prevent the toes dragging on the ground.
Conclusion
In those patients where arthrodesis is indicated, the vast majority benefit from surgery. Fusion of a joint is undoubtedly a major undertaking, and these procedures are commonly performed by specialist orthopedic surgeons. We will be pleased to give as much help and support as possible if you decide to give your pet the opportunity of arthrodesis surgery.
Pet of the month – May 2019
by admin on April 30th, 2019
Category: Pet of the Month, Tags:
Pet of the Month is Scooby, an elderly Springer Spaniel, seen here having Acupuncture.
Scooby suffers from arthritis of various joints and lumbosacral disease, and is on appropriate pain medication. The acupuncture stimulates anatomical points of the body and prompts the body to produce chemicals that decrease painful sensations. This is Scooby’s third weekly session and he is showing some slight improvements. He also quite enjoys it!
Pet of the month – April – Molly
by admin on April 2nd, 2019
Category: Pet of the Month, Tags:
What is Diabetes Mellitus (Sugar Diabetes)?
Most of the food that animals eat is turned into sugars to provide energy for the body. The sugar in the blood then needs to get into the cells of the body to help them work. A hormone called insulin, which is produced by the pancreas (an organ in the tummy near the stomach), helps the sugar to get into the cells. Diabetes develops when the body does not produce sufficient insulin. Insulin regulates blood sugar levels, and when the insulin levels are too low, blood sugar (glucose) levels increase, resulting in diabetes. Diabetes is a potentially life threatening illness, but fortunately it is one which we are able to treat successfully in the majority of cases.
Diabetes occurs most commonly in older dogs, and in middle-aged overweight cats. Some dogs and cats develop diabetes when they are younger, because they have a genetic predisposition for the condition.
What are the signs of Diabetes?
- Increased thirst
- Increased frequency and/or volume of urination
- Possible increased appetite
- Possible weight loss
- Possible smelly urine – because of the presence of ketones (see below) or infection
- Possible lethargy/tiredness
How is Diabetes treated?
Diabetes is best treated with insulin. In most cases, insulin is administered as an injection under the skin twice a day.
Ketoacidosis is a potential complication of Diabetes. In cases of uncontrolled diabetes, toxic (poisonous) metabolites (natural break-down chemicals) are produced which can lead to illness, lethargy, coma and death.
In Molly’s case we believe that her diabetes became unstable when she came into season, due to her altered hormonal levels, and we hope to spay her at an appropriate time in the near future.
Following intensive care Molly has substantially improved and her diabetes is being more effectively controlled with the use of a Flash monitoring system (Freestyle Libre).
A flash glucose monitoring system measures sugar (glucose) levels continuously throughout the day. It can help your diabetes team see:
- if sugar levels are going up or down
- how sugar levels change over time
- the past 8 hours so you can see what happens overnight
Flash does not actually measure blood sugar levels. It measures the amount of sugar in the fluid under your skin, called interstitial fluid. Interstitial fluid sugar readings are a few minutes behind your blood sugar levels.
The measurements can help your vet team make decisions about treatment and any adjustments you need to make.
A flash system is made up of:
- a sensor which is stuck to the body (about the size of a £2 coin)
- a reader – a small device you use to scan the sensor to see your pet’s sugar levels
You can also use a smartphone app to scan the sensor.
Sensors usually last for 14 days.
Corneal Sequestrum
by admin on April 2nd, 2019
Category: News, Tags:
What is the cornea?
The cornea is the clear window of the eye. It is a very delicate structure which is less than a millimetre thick. In order to be transparent, the cornea has no blood vessels. This makes the cornea vulnerable to injury and infection, and results in a slow healing response to deep wounds.
What is a corneal sequestrum?
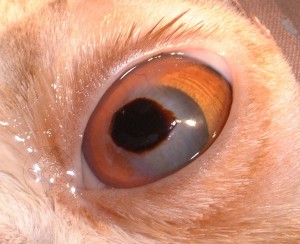
A corneal sequestrum is a part of the cornea which has died off and which is then rejected by the remaining healthy cornea. Most sequestra (as more than one sequestrum is known) affect the centre of the cornea. Corneal sequestra are usually pigmented in different shades of brown and may vary in appearance from subtle bronze staining to very obvious dark plaques. In some patients, blood vessels grow into the cornea in response to the sequestrum and a reddish rim may surround the pigmented plaque. In many affected patients, their tears will also be darkly pigmented and brown to black discharge may crust on the eyelids.
Is a corneal sequestrum a problem for affected cats?
Overall, the answer to this question is yes. In their very early stages, corneal sequestra will not cause pain or visual impairment but with time corneal ulceration (wounding) develops, and patients will show intermittent signs of eye pain such as blinking, squinting, weeping and light-shyness. Occasionally patients will show signs of a sequestrum only after several episodes of apparently spontaneous corneal ulceration.
Corneal sequestra can become infected, and this may lead to loss of the eye in the absence of rapid treatment.
What causes a corneal sequestrum?
Chronic injury has been identified as a possible cause of sequestrum formation and especially abnormalities of the eyelids such as inward turning of the eyelids and eyelashes. However, even today, it is not known why the majority of patients develop corneal sequestra. Many theories have been investigated and herpesvirus (one of the cat flu viruses) has been identified as a possible cause in crossbred (domestic short haired) cats. However, most corneal sequestra are seen in purebred cats such as Persians and British Short Hair cats. It is possible that the special shape of the faces of these patients is associated with the problem. They generally have big bulging eyes which often have a poor blinking response. Herpesvirus does not generally appear to be related to sequestrum developments in purebred cats. Abnormalities of the tear film such as a poor quality or quantity of tears are also considered to be involved in some cases.
What treatment options are available if my cat has a corneal sequestrum?
There are three major treatment options available:
- Conservative treatment with antibiotic and lubricating ointments to reduce irritation and prevent infection until the eye has shed the sequestrum by itself.
- Surgical excision of the sequestrum and placement of a soft contact bandage lens.
- Surgical excision of the sequestrum followed by a grafting procedure to provide support for the affected area of cornea and to reduce the risk of the sequestrum coming back.
In general, it is unlikely that continued conservative treatment will be recommended, as this is usually associated with prolonged periods of eye pain for the patient. Furthermore, ongoing monitoring and veterinary care will be required to try and reduce the risk of infection or rupture (bursting) of the cornea. This is a risk as the sequestrum may spread deeper. The cost advantage of not proceeding with surgery usually does not outweigh the prolonged care and discomfort for patients suffering a sequestrum, and the result of surgery may be less good with later intervention.
In our experience, surgical removal of the corneal sequestrum under the operating microscope is the treatment of choice. Given the depth of the lesion and the risk of retention of some pigment in the cornea after surgery, an additional grafting procedure may well be recommended.
Grafting procedures involve the placement of a piece of conjunctiva (the lining of the white of the eye) or other tissue into the wound following excision of the sequestrum. Grafts are usually stitched into place and will lead to a partial impairment of corneal transparency. However, the eye should still retain useful vision.
What does surgery for sequestrum removal involve?
Removal of corneal sequestra is carried out under general anaesthesia with the help of the operating microscope. The area around the eye is clipped. During the anaesthetic, the patient’s heart rate, blood pressure and blood oxygen concentration are monitored and a fluid infusion is given intravenously to maintain good blood circulation. Once the sequestrum has been removed, the surgeon will usually either place a contact lens or place a graft (see previously mentioned). Following the surgery, the operated eye is likely to be slightly sore and many cats will only partially open it for a few days.
What aftercare will be required?
Post-operatively, the patient needs to wear an Elizabethan collar to prevent damage to the wound by rubbing or scratching. Gentle cleaning of the operated eye with wet cotton wool twice daily is recommended.
An antibiotic ointment is generally applied to the eye for approximately ten days post-operatively. A short course of antibiotic tablets and painkillers may also be given after surgery. The use of false tears or other lubricant preparations may be recommended long-term in some cases, usually to be applied once or twice daily.
How successful is surgery for removal of a corneal sequestrum?
Surgical removal of corneal sequestra is a very successful surgery in uncomplicated cases.
The main risks of the procedure are wound infection and loosening of the graft. On occasion, a second procedure may be required to achieve a satisfactory result. Fortunately, the loss of an eye due to complications or progression of the disease after surgical sequestrum removal is very rare.
Surgery for sequestrum removal and placement of a graft aims at reducing the risk of sequestrum recurrence but cannot guarantee that the same eye will never be affected with another sequestrum.
Can my own veterinary surgeon remove the corneal sequestrum?
Removal of a corneal sequestrum is a procedure that requires a skilled and experienced micro-surgeon, equipment for magnification and illumination, and fine surgical instruments that will not damage the delicate tissues of the eye. For this reason most general practitioners will recommend referral to an ophthalmic specialist for treatment of this condition.
Do I have to return to the eye specialist for the aftercare?
After an eye has developed a serious disease which has required a major procedure, it is best to have its progress checked by the specialist. The number of revisits will depend upon the severity of the problem and the post-operative progress. In many cases only two or three re-visits will be required. In more complex cases there may be a need to continue with further check-ups from time to time.
Is my cat’s other eye at risk?
Unfortunately, the other eye is also at risk of sequestrum formation and must be carefully monitored for this reason. At the moment no treatment is known that will reliably prevent sequestrum formation, but the use of ocular lubricants may be helpful in providing some degree of additional corneal protection.