News
Pet of the month – April 2020
by admin on April 6th, 2020
Category: Pet of the Month, Tags:
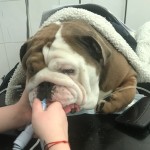
This delightful 4 year old Bulldog first came to see us having been very sick. Buzz was also straining to urinate.
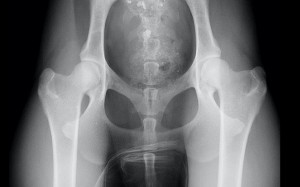
An ultrasound scan showed he had numerous stones in his bladder, necessitating urgent surgery.
Surgery proved more extensive than expected as Buzz not only had 50 stones in his bladder but he also had 18 stones wedged tightly in his urethra, the tube connecting the bladder to the outside world. His bladder had to be opened and evacuated and his urethra had to be incised on the underside of his penis to release the obstacles.
Buzz is recovering really well and we are extremely pleased with his progress to date!
COVID-19 UPDATE & FAQ’s
by admin on April 6th, 2020
Category: News, Tags:
Firstly may we say a massive thank you to all our customers for being so understanding and accommodating at this difficult time.
And a huge thank you to all our amazing vets, nurses and receptionists for pulling together to find the best possible means by which to provide local pets with the care they need.
Small teams are working 24/7 on a roster to provide emergency care and urgent treatment where animal welfare would be compromised by delay.
Our main Littlehampton hospital REMAINS OPEN however as you would expect we have put in place all the necessary steps to ensure that we reduce the risk of virus transmission, and are keeping the main door closed. We need to keep everyone safe.
Concerned about your pet’s health but don’t think it’s an emergency?
If you are worried about your pet, phone us and explain your situation. We’ll arrange a suitable way of conducting your appointment that is in everyone’s best interests.
There are a variety of options available to everyone – the important thing is to let us know and we’ll work together!
To respect social distancing rules, we are replacing our standard consultation service with video and telephone consultations. Please contact the practice to arrange an appointment and discuss suitable communication platforms (eg Skype, Facetime, WhatsApp). Payment can be made over the phone.
What constitutes an emergency that needs immediate care?
If any of the below apply to your pet, contact us IMMEDIATELY:
- Breathing difficulties
- Open wound injuries
- Trauma (e.g. car accidents)
- Male cats struggling in the litter tray to pass urine
- Rabbits neglecting food
- Swallowing hazards ie.toys/clothes
- Ingestion of poisonous/harmful substances
- Eye problems
- Vomiting or diarrhoea especially if your pet appears quiet or depressed or if it is going on for a long time (more than 24 hours)
- Swollen abdomen or retching (especially large dogs)
- Loss of thirst & appetite
- Struggling to give birth
- Seizuring/fitting
- Collapse
If the recommendation is to come into the practice, please follow the advice given by our staff.
- We will ask that you telephone us when you arrive in the car park.
- A member of staff will come out and take your pet into the clinic.
- After making an assessment we will ring you on your mobile to discuss the necessary treatment and way forward.
COVID-19 FAQ’s
Can I bring my pet in for an INITIAL VACCINATION COURSE?
A vaccination is not deemed an emergency and we will not be offering an initial vaccination course. If you have a puppy, we recommend that they are kept inside and not exposed to other dogs. You should book a vaccination course as soon as possible after normal service resumes.
We will review this and provide a further update if the government extends the initial three weeks of enhanced measures to slow the spread of the virus.
Can I bring my pet in for their ANNUAL VACCINATION BOOSTER?
We can postpone this vaccine for up to 3 months after the due date without requiring a restart. During these exceptional times, we ask that you delay the booster until up to a maximum of 3 months after the due date.
Can I bring in my pet for a HEALTH CHECK?
Not at this moment in time because this is not deemed critical. However, if your pet is ill we will be able to conduct a consultation via a video or telephone consultation. Please ask the practice for further information.
Can I bring my pet in for NAIL CLIPS? Or to have their ANAL GLANDS expressed?
This should be postponed if your pet is not in any danger of feeling discomfort. If you are uncertain whether this is the case, please arrange a video or telephone consultation with the vet.
How can I get my REPEAT FOOD or MEDICATIONS?
It is important that you continue to give your pet the appropriate food and medication. We are looking at ways of getting these to clients who are due them and postal / delivery services may be an option. Please contact us to make suitable arrangements.
How can I get my FLEA, WORM, TICK and FLYSTRIKE treatments?
It is important that you continue to give your pet the appropriate treatments. We are looking at ways of getting these to clients who are due them and postal / delivery services may be an option. Please contact us to make suitable arrangements.
Can my pet still have ELECTIVE OPERATIONS such as Neutering and Lumps removals?
These operations are not deemed to be critical during these extraordinary times and we therefore ask that you postpone these procedures, until government guidelines on social distancing change.
What about ULTRASOUNDS and BLOOD TESTS?
It depends whether these are deemed critical or not – please contact us to discuss.
Hip dysplasia
by admin on March 3rd, 2020
Category: News, Tags:
What is hip dysplasia?
Hip dysplasia means abnormal development of the hip joint. It inevitably leads to the development of arthritis (osteoarthritis). Either the hip dysplasia or the secondary arthritis may cause hip pain.
Hip dysplasia is a genetic disorder caused by the combination of genes from the parents (dam and sire). During the first few months of life, as the hips are developing, they become unstable. As a result the ball (femoral head) and socket (acetabulum) move apart during weight bearing. This causes abnormal forces on the soft bones which leads to the ball becoming flattened and the socket becoming shallow. The process is self-perpetuating and causes damage to the covering of the bones (the articular cartilage). Cartilage damage is a key feature of the secondary osteoarthritis.
What are the signs of hip dysplasia?
Hip dysplasia is a common condition, especially in large breed dogs. The key signs are hind limb lameness and stiffness. The latter is generally most evident after rest following exercise. Difficulty rising and reluctance to jump or exercise are also common features. A rolling hind limb action may be seen in young dogs. More subtle signs include restlessness, moaning and licking the skin over the hip.
Signs tend to develop when the dog is immature and growing (five to 10 months of age) or when adult (perhaps a few years of age). When immature, it is the instability of the hip that causes the pain whereas in adult dogs it is the osteoarthritis which results in discomfort.
How is hip dysplasia diagnosed?
Examination may reveal muscle wastage (atrophy), especially over the hips. Manipulation of the joints may cause increased pain and instability may be palpable.
X-rays (radiographs) are necessary to diagnose hip dysplasia. They enable the severity of the abnormal joint development and presence of secondary osteoarthritis to be assessed.
How can hip dysplasia be treated?
The majority of dogs with hip dysplasia can be managed satisfactorily without the need for surgery. Exercise often needs to be controlled to some degree. Each dog will have its own threshold of duration and type of activity beyond which hip pain may increase. Hydrotherapy is often beneficial. Dogs that are overweight benefit from being placed on a diet. Tit-bits may need to be withdrawn and food portions reduced in size. Regular monitoring of weight may be necessary. Painkillers (anti-inflammatory drugs) may be indicated to make the dog more comfortable. Long-term drug therapy should be avoided if at all possible in view of potential side effects.
Some dogs with hip dysplasia fail to respond satisfactorily to conservative treatment and in these cases surgery may be indicated. The two key types of surgery are (1) reconstructive and (2) salvage.
Reconstructive surgery
In some young dogs (usually less than a year of age) the abnormal hip joint may be reconstructed to make it more stable. This involves cutting the pelvis and rotating the cup (acetabulum) over the ball (femoral head). The rotated section is secured in the new position with a specially designed plate. Either a triple pelvic osteotomy (TPO) or a double pelvic osteotomy (DPO) can be performed. Reconstructive surgery has the advantage of maintaining the dog’s own joint tissues and hopefully reducing the development of osteoarthritis. Unfortunately many young dogs with hip dysplasia are not good candidates for reconstructive surgery.
The aftercare following DPO or TPO surgery is very important. Exercise has to be restricted for eight weeks until the cut bones heal. Long-term hip function is generally good. Further surgery or long-term medication is generally not necessary.
Salvage surgery
Adult dogs with hip dysplasia and secondary osteoarthritis that fail to respond to medical management may require salvage hip surgery. The principle options are to replace the hip with an artificial one (total hip replacement) or to remove the ball (femoral head removal or excisional arthroplasty).
Total hip replacement generally results in significantly better limb function compared to femoral head removal and the recovery is much quicker. However, although uncommon, there are potential complications with total hip replacement surgery that need to be carefully considered prior to making a decision. With modern systems total hip replacement can be performed successfully in all sizes of patients.
Femoral head removal provides a ‘false joint’ where the limb is supported on the pelvis by scar tissue and the surrounding muscles. Recovery following surgery is slow and the limb ends up slightly shorter. Aftercare, especially physiotherapy and hydrotherapy, is very important.
Total hip replacement
Total hip replacement surgery involves replacing the painful joint with a plastic cup and a metal ball (acetabular and femoral prostheses). Care following surgery is critical to reduce the possibility of complications, such as dislocation of the prostheses. A rapid reduction in joint pain and improvement in limb function are to be expected.
What is the outlook with hip dysplasia?
The outlook or prognosis with hip dysplasia and the associated osteoarthritis is generally good. As mentioned above many dogs can be managed successfully with conservative treatment involving modification of exercise and weight, with or without the need for anti-inflammatory painkiller drugs. Those that fail to respond satisfactorily may necessitate reconstructive procedures (DPO or TPO) or salvage surgery such as total hip replacement. The outcome of these procedures is generally very good, albeit that there are potential complications.
Pet of the month – March 2020
by admin on March 3rd, 2020
Category: Pet of the Month, Tags:
Pet of the month for March is Boots, a delightful one year old Whippet who was recently hit by a car.
Boots presented with severe difficulty breathing and respiratory distress. Radiography showed he had a pneumothorax, which is an accumulation of air outside the lungs, but inside the chest wall. The air outside the lung prevents the lungs from inflating normally, and as happened with Boots can lead to lung collapse.
Treatment involved draining the air from inside the chest cavity to allow the lungs to expand, and oxygen therapy was provided until Boots was stable. Additonally strong pain relief was provided.
Boots required intensive care and repeated chest drainage until the damage repaired.
We are delighted to report that Boots is now back to good health!
Pet of the month – February 2020
by admin on February 3rd, 2020
Category: Pet of the Month, Tags:
She is seen here recovering from surgery to take skin biopsies, required during the investigation of her ongoing dermatitis, an issue which started when she was just 5 months old.
The recurring scabs and spots on Frida’s head and neck proved unresponsive to treatment so she was referred to a skin specialist who came to our clinic especially to see Frida. We hope the results will provide clarity on the cause of Frida’s condition and the best way of managing and or curing it.
Asthma and Bronchitis in Cats
by admin on February 3rd, 2020
Category: News, Tags:
What is asthma and feline bronchitis?
Asthma is a common respiratory condition in cats. The disease is caused by activation of inflammation in the lungs in response to irritants or allergens in the environment. The cells in the lungs respond by increased production of mucus and reversible narrowing (spasm) of the small airways. The condition is similar to the well described human form of the disease. In most cases the exact cause or trigger is unknown. A similar condition exists called chronic bronchitis. This shares many similarities with asthma. In cats with chronic bronchitis inflammation of the small airways is present however the reversible spasm is not.
What are the signs?
The signs of both conditions are similar and can vary in severity and frequency. The most common include:
- Coughing
- Rapid breathing/open-mouth breathing
- Increased noise or wheezing sounds when breathing
- Breathing difficulties/increased effort whilst breathing
Some cats can have a sudden life-threatening asthma attack. The signs of this would include breathing difficulties, open mouth breathing and weakness/collapse. This can happen in cats with previously diagnosed asthma or can be the first sign in some cases. Immediate veterinary attention is required in any cat with these signs at home.
How are the conditions diagnosed?
A diagnosis of asthma or chronic bronchitis is normally reached after a series of diagnostic tests. Often these are performed to exclude other causes of coughing/breathing difficulties in cats. Firstly a thorough history is taken. A physical examination is then performed. Harsh or wheezy sounds can be heard when the chest is auscultated.
In addition a combination of some or all of the following tests can be performed:
- Blood tests to assess general health and to evaluate white blood cell number and type.
- Faecal tests to check for feline lungworm infection may be performed.
- X-rays or a CT scan of the chest. In some asthmatic cats X-rays and/or CT scan can be normal. In others thickened airway walls are seen or signs of ‘over-inflation’ of the lungs. These tests are also important to rule out other causes of coughing/breathing abnormalities in cats.
- Bronchoscopy or video camera into the lungs to examine the inner lining of the airways.
- An airway wash may be performed. The fluid is then examined under the microscope to check inflammatory cell type and number and whether there is any evidence of bacteria or parasites. In addition the fluid is often cultured and a test for bacterial and/or parasitic DNA performed.
What is the treatment?
Both conditions are treated with anti-inflammatories (normally corticosteroids). Generally the medication is administered in one of three ways
- By injection: in cats which are hospitalised short-acting injectable forms of steroids may be administered, especially in patients that are experiencing breathing difficulties. Rarely long-acting injectable forms that can last between 3-6 weeks can be used in patients who cannot be given medication by mouth or inhaled medication.
- By mouth (tablet or occasionally liquid form): to begin with a higher dose is used before gradually reducing to the minimum effective dose.
- By inhalation: metered dose inhalers (MDIs) can be used as an alternative to oral medication. These are administered using a spacer device attached to a specially designed face mask for cats. Once a cat has become accustomed to the device it is normally well tolerated.
The advantage of this method of administration is that the steroids are delivered directly to the lungs and absorption to the rest of the body is minimised. This can reduce systemic side effects associated with oral steroid therapy. Further information regarding the Aerokat™ spacer device including a video demonstrating how it is used can be found on the following website: https://www.trudellmed.com/
In addition some cats require bronchodilators which are drugs that can help to relax (or dilate) the small airways. This medication can be given by injection in patients that are hospitalised or by mouth (tablets) at home. Inhaled bronchodilators are also available.
What is the prognosis for feline asthma?
With appropriate treatment the prognosis is normally good. Many cats will require life-long therapy. Unfortunately some cats can have progressive signs despite treatment. Uncommonly in some asthmatic cats a severe attack can be fatal.
If you have any questions about your cat’s condition, or his or her treatment, please do not hesitate to contact us.