News
Archive for the ‘News’ Category
Canine Flank Alopecia
by admin on October 1st, 2019
Category: News, Tags:
What is canine flank alopecia?
Canine flank alopecia is a localised, often cyclic, disease of the hair follicles resulting in hair loss over the flanks of affected dogs. It is also known by the names cyclic flank alopecia, recurrent flank alopecia and seasonal flank alopecia, but these terms are not always accurate as the condition can appear at various times of the year, vary in duration, be continuous or be sporadic in nature.
What causes flank alopecia?
The cause of this condition is not known. However, as hair loss often occurs at times of the year when day length is at its shortest, light exposure may be involved. The mechanisms by which this might occur are not understood at present.
What are the clinical signs?
Canine flank alopecia occurs in dogs with ages ranging from 1 year to 11 years, although most cases develop between 3 and 6 years. This condition is seen more commonly in breeds such as Boxers, Airedale terriers, English Bulldogs and Schnauzers.
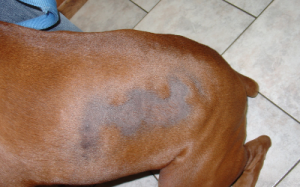
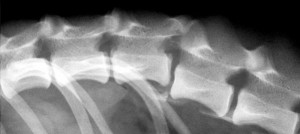
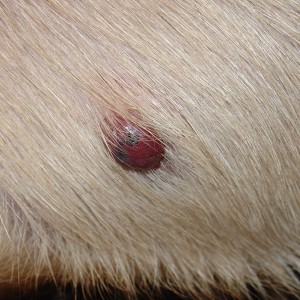
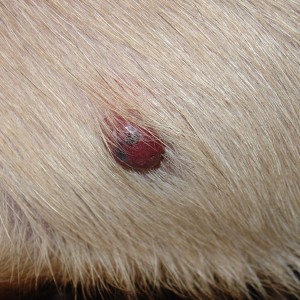
The condition causes areas of non-itchy hair loss over the flanks of affected dogs (Figure 1). The skin at the affected sites usually appears normal, although it often becomes very dark with pigmentation, and hair re-growth of a different colour sometimes occurs. Surrounding hair and skin is usually normal. Canine flank alopecia can occur on both sides of the dog or be limited to one side, and hair loss can also occur over the base of the back (Figure 2). The disease in some dogs is cyclic, with hair loss occurring at the same time each year and hair re-growth occurring in the times between. In other dogs, hair loss is more permanent, and no re-growth is seen following the initial loss. Some dogs are reported as only having one cycle of hair loss and re-growth in their lives.
How is it diagnosed?
The diagnosis of canine flank alopecia can often be made based on the clinical findings, since the lesions are so striking. Some hormonal diseases of dogs can present with non-itchy hair loss, so blood and urine tests may be warranted if there is a concern about these diseases.
Additionally, biopsies of affected skin can be taken which are then sent off for analysis at a laboratory. Biopsies can be supportive of a diagnosis of canine flank alopecia.
What are the treatments available?
Canine flank alopecia is a cosmetic disease. As dogs remain healthy, with many re-growing their hair eventually, a decision not to treat the affected dog is often taken.
If treatment is requested, melatonin is generally considered the treatment of choice as it is relatively safe and inexpensive. It is difficult to judge the response to medication though due to the high rate of spontaneous hair re-growth.
What is the outlook/prognosis?
The prognosis for this cosmetic disease is good, with dogs remaining systemically healthy despite unpredictable hair growth. The prognosis for full and normal hair re-growth at affected sites is also often good, but the disease is highly variable.
Nasal Disease
by admin on September 2nd, 2019
Category: News, Tags:
What diseases can affect the inside of the nose?
There are several different types of problem that can affect the nasal cavity of dogs and cats. The most common conditions in dogs include inflammation of the nasal cavity (rhinitis) and nasal tumours (cancer). Rhinitis in dogs can be due to a number of problems including allergy (called lymphoplasmacytic rhinitis), fungal infection (most commonly a fungus called Aspergillus) and foreign bodies (such as grass blades). In cats fungal disease is rare, whilst polyps (benign outgrowths of tissue) in the nose/ throat, rhinitis of unknown cause and tumours are more common. Bacterial infection can occur as a consequence of the underlying disease but does not cause nasal disease by itself.
What are the signs of nasal disease?
- Sneezing
- Snorting
- Nasal discharge
- Nose bleeds
- Nasal pain
- Nasal ulceration or loss of pigment around the nostrils
- Reverse sneezing (this can look like spasms of choking or difficulty breathing and can be quite disturbing to see but is not a life threatening problem)
How is nasal disease diagnosed?
Bloods tests may be performed as part of an initial investigation, looking at general organ health prior to performing an anaesthetic or other tests. Sometimes blood tests are performed to look at how well the patient’s blood is clotting in patients with nose bleeds. Most commonly X-rays or a CT scan of the nasal cavity are performed under general anaesthesia and a procedure called rhinoscopy is carried out, in which an endoscope camera is inserted up the nose or used to look at the back of the throat.
Nasal X-rays may show damage to the small bones in the nose and they may reveal the presence of fluid or tumours. X-rays can sometimes look normal even when nasal disease is present, however.
A CT scan is a much more effective and sensitive way of detecting disease in the nose and will not uncommonly reveal abnormalities that haven’t shown up on an X-ray. A CT scan will also help to define the extent of any damage or the location of a tumour.
Rhinoscopy (passing a small camera inside the nose) is performed to look for abnormalities including fungal infection, tumours, and foreign bodies and to help take a tissue biopsy from the nose to send for analysis.
How is nasal disease treated?
The treatment for nasal disease depends upon its underlying cause and severity. Sometimes medication in the form of tablets is prescribed; anti-fungal solution must be put into the nose or the sinuses to treat the fungal infection Aspergillus, whilst either radiation therapy or chemotherapy may be required for the treatment of nasal tumours.
What is the long term outlook (prognosis)?
The long term outlook depends upon the underlying disease. Patients usually recover well from removal of a foreign body. Allergic rhinitis is not a life-threatening problem, but treatment is generally aimed at controlling rather than curing the problem and some patients may not respond as well as would be hoped. Aspergillus can respond well to therapy, but the condition may be recurrent and difficult to cure in some patients.
More specific advice and guidance about treatment of nasal disease for individual patients can be given once the diagnosis has been made and detailed information has been obtained from the diagnostic work-up.
Spinal Fractures
by admin on August 1st, 2019
Category: News, Tags:
Spinal Fractures
Fractures (breaks) of the spine occur when dogs and cats are involved in road traffic accidents or suffer other major trauma such as a fall or running into a patio door. Spinal fractures are often associated with varying degrees of injury to the spinal cord (the bundle of nerves inside the vertebrae) and, therefore, nerve damage. Although many animals may be paralysed as a result of the fracture, they will often recover, provided that they retain the ability to feel pain and that they are managed appropriately. Some cases can be treated medically, but it is often necessary to consider surgery to stabilise a fractured spine.
What is involved in a spinal fracture?
In a spinal fracture, the bones (vertebrae) of the spine break (fracture) or come apart from each other (dislocate or luxate). Fracture of the spine usually occurs as a result of a significant injury, such as being hit by a car, although occasionally the bones in the spine may fracture with minimal, if any, trauma because they are already weakened by a condition such as a tumour (referred to as a ‘pathological fracture’).
When the vertebrae of the spine fracture or dislocate (luxate) the associated vertebral displacement often injures the nerves of the spinal cord. The concussion and compression of the spinal nerves affects nerve function, and the signs that develop may vary from only mild weakness through to paralysis (inability to voluntarily move the limbs). Severely affected patients may become incontinent and lose the ability to feel pain in their limbs and tail.
How are spinal fractures diagnosed?
Physical examination of the patient by the specialist may enable detection of instability of the spine or abnormal alignment of the spine. Importantly, examination also enables assessment of the severity of any associated spinal cord injury – in particular, whether or not the patient can still feel pain.
X-rays (radiographs) are often obtained to look for evidence of fracture (or luxation) of the vertebrae and are generally sufficient to make a diagnosis in the majority of cases. Occasionally a more advanced imaging technique is preferred, to provide additional detail of the spine. CT scanning is particularly good at looking at the bony detail of fractures which may not be apparent on normal X-rays. MRI scanning is not so good at detecting damage to bones of the spine, but it is excellent for assessing any damage to the spinal cord.
How are spinal fractures managed?
Spinal fractures (and luxations) are often emergencies because of the associated spinal cord injury and risk of further damage. As a result, they need to be treated with the minimum of delay. Affected dogs and cats are often in significant pain, and care should be taken to avoid the handler being bitten or scratched. Patients should be moved with great caution in case the spine (vertebral column) is unstable, as further movement may aggravate the injury and any nerve damage. Strapping the patient to a rigid board may be helpful in some cases.
Some fractures of the spine may be treated conservatively without the need for surgery. This is particularly appropriate in patients with relatively stable vertebrae and minimal spinal cord injury. Conversely, dogs and cats with unstable fractured spines, those with significant spinal cord injuries and those in severe pain are often best treated surgically. Surgery aims to re-align and stabilise the affected vertebrae. The procedure most often involves placing screws or pins in the bones on either side of the fracture (or luxation) and securing them with either a plate or cement.
What is the outlook (prognosis) in patients with spinal fractures?
The outlook in dogs and cats with spinal fracture is primarily dependent on the severity of the spinal cord injury and how the patient is treated. Provided the ability to feel pain in the limbs and tail is maintained and the patient is managed appropriately, the outlook is generally good. Recovery may take a number of weeks (or even months in severely affected cases) and supportive care, including physiotherapy/hydrotherapy exercises, may be necessary. In contrast, patients with spinal fractures that can no longer feel pain are very unlikely to recover, no matter how they are treated, since the spinal cord injury is generally severe and irreversible.
Pancreatitis in Dogs
by admin on July 3rd, 2019
Category: News, Tags:
What is pancreatitis?
The pancreas is an organ in the abdomen (tummy) which is responsible for releasing enzymes (types of proteins) to digest food. The pancreas also releases important hormones (such as insulin) into the bloodstream. Pancreatitis occurs when the pancreas becomes inflamed (tender and swollen). In most cases pancreatitis occurs for no apparent underlying reason, although sometimes it can have a particular cause (such as scavenging food). Pancreatitis most commonly affects middle aged to older dogs, but in addition, dogs of certain breeds (e.g. Cocker Spaniels and Terrier breeds) are more prone to developing the condition.
What are the signs of pancreatitis?
Pancreatitis can cause a variety of symptoms, ranging from relatively mild signs (e.g. a reduced appetite) to very severe illness (e.g. multiple organ failure). The most common symptoms of pancreatitis include lethargy, loss of appetite, vomiting, abdominal pain (highlighted by restlessness and discomfort) and diarrhoea.
How is pancreatitis diagnosed?
The possibility that a dog may be suffering from pancreatitis is generally suspected on the basis of the history (i.e. loss of appetite, vomiting, etc) and the finding of abdominal pain on examination by the veterinary surgeon. Because many other diseases can cause these symptoms, both blood tests and an ultrasound scan of the abdomen are necessary to rule out other conditions and to reach a diagnosis of pancreatitis. Although routine blood tests can lead to a suspicion of pancreatitis, a specific blood test (called ‘canine pancreatic lipase’) needs to be performed to more fully support the diagnosis. An ultrasound scan is very important in making a diagnosis of pancreatitis. In addition, an ultrasound scan can also reveal some potential complications associated with pancreatitis (e.g. blockage of the bile duct from the liver as it runs through the pancreas).
How is pancreatitis treated?
There is no specific cure for pancreatitis, but fortunately most dogs recover with appropriate supportive treatment. Supportive measures include giving an intravenous drip (to provide the body with necessary fluid and salts) and the use of medications which combat nausea and pain. Most dogs with pancreatitis need to be hospitalised to provide treatment and to undertake necessary monitoring, but patients can sometimes be managed with medication at home if the signs are not particularly severe. At the other extreme, dogs that are very severely affected by pancreatitis need to be given intensive care.
One of the most important aspects of treating pancreatitis is to ensure that the patient receives sufficient appropriate nutrition while the condition is brought under control. This can be very difficult, because pancreatitis causes a loss of appetite. In this situation it may be necessary to place a feeding tube which is passed into the stomach, and through which nutrition can be provided. If a dog with pancreatitis is not eating and will not tolerate a feeding tube (e.g. due to vomiting), intravenous feeding (using a drip to supply specially formulated nutrients straight into the bloodstream) may be necessary.
What is the outcome in pancreatitis?
It may be necessary for dogs with pancreatitis to be hospitalised for several days, but fortunately most patients with the condition go on to make a complete recovery, provided that appropriate veterinary and nursing care is provided. In some instances, dogs can suffer repeated bouts of the condition (called ‘chronic pancreatitis’) and this may require long term management with dietary manipulation and other approaches which the specialist will discuss with you in detail, as required.
Inflammatory Bowel Disease (IBD)
by admin on June 6th, 2019
Category: News, Tags:
What is IBD?
IBD is a disease that causes inflammation in any part of the digestive tract (stomach and/or intestines and/or colon i.e. large bowel). Some breeds of dog, such as Soft Coated Wheaten Terriers have a genetic predisposition to this disease. In other breeds of dogs and cats it can be triggered by a parasite or food intolerance. More commonly no specific underlying cause is found and the disease is thought to be caused by an over-activity of the body’s immune system (which normally fights off infections) to ‘foreign’ proteins (such as food) that are eaten, resulting in inflammation.
What are the signs of IBD?
- Weight loss
- Vomiting
- Diarrhoea
- Increased or decreased appetite
- Blood or mucus in the faeces
How is IBD diagnosed?
IBD is diagnosed by a combination of tests, as several other diseases can cause similar signs. Blood tests are often performed to rule out other underlying diseases such as liver or kidney disease, and faecal examination is performed to look for any parasites. Cats with IBD can have low vitamin B12 levels therefore vitamin B12 is measured in all cats.
As foreign body obstructions, or sometimes tumours, can cause weight loss and vomiting, X-rays or ultrasound scans are usually performed to rule out these problems.
Finally, the ultimate diagnosis of IBD is made by taking biopsies from the stomach, intestine or colon. Usually this is performed under a general anaesthetic using a flexible endoscope camera, of which we have several different sizes to suit different sizes of patient. This is not an invasive procedure and most pets recover very quickly and will go home within 24 hours.
How is IBD treated?
Many dogs and cats will improve following a dietary trial. Often this involves prescribing a new diet that is hypoallergenic (i.e. unlikely to cause a reaction) or contains a protein source that your pet has not eaten before (such as venison or salmon). This is fed for 1 to 2 months and it is very important that no other food, treats or tit-bits are given. Some pets won’t respond to one diet but will respond to an alternative diet.
Pets that don’t respond to diet alone may be prescribed certain antibiotics.
Dogs and cats that are severely affected or that don’t respond to the treatments mentioned above will be prescribed steroids. A high dose is prescribed initially and this is decreased every few weeks for several months. Sometimes in pets that don’t tolerate steroids or don’t respond to steroids alone, other drugs which suppress the immune system are prescribed.
What is the long term outlook? (prognosis)?
IBD has a broad spectrum of severity, ranging from mild vomiting and diarrhoea to severe weight loss and fluid build up in the abdomen. It is not generally a life-threatening disease but can be in severely affected patients. It is not a curable disease, therefore the aim of treatment is to minimise the frequency of vomiting and diarrhoea: it is rare to be able to stop the clinical signs altogether. Keeping a diary of how often the signs are happening can be helpful to us in establishing the success of treatment. Most dogs and cats are able to live a good quality of life following a diagnosis of IBD.
Arthrodesis
by admin on April 30th, 2019
Category: News, Tags:
What is arthrodesis?
Arthrodesis means the surgical fusion of a joint. In other words, the bones forming the joint are permanently joined together so that there is no movement in this part of the limb. Arthrodesis is a salvage procedure that is generally only performed when there are no other options to save the function of the joint.
What joints can be arthrodesed (fused)?
The shoulder, elbow, carpal (wrist), stifle (knee), hock (ankle) and digit (toe) joints can be arthrodesed. The main joint that cannot be fused is the hip joint. This is generally not a problem since the hip joint can be replaced with an artificial one. Elbow and knee replacements are also possible alternatives to arthrodesis of these joints.
Reasons for performing an arthrodesis
The principle indications for arthrodesis are:
- osteoarthritis that is causing chronic pain and cannot be managed medically
- joint instability that cannot be treated by other means
- fractures involving the joint surface that cannot be repaired
- infection involving the joint that fails to respond to antibiotics
- tumours in or around joints
- muscle/tendon rupture that cannot be managed directly
What does arthrodesis involve?
There are a number of important steps when fusing a joint:
- the surface of the joint (known as the articular cartilage) must be removed to enable bony fusion.
- a bone graft should be placed into the spaces between the bones to promote fusion. This may be an autograft (from the patient), an allograft (from a donor) or a combination of both.
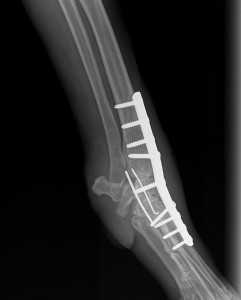
- the bones forming the joint to be arthrodesed must be rigidly stabilised to maximise the possibility of bony fusion. This is most commonly achieved with one or two plates that are secured to the bones under the skin. Occasionally an external skeletal fixator (a metal framework) is employed, where the bones are stabilised with pins that penetrate the skin and are attached to bars on the outside of the limb.
- exercise must be restricted until there is radiographic (X-ray) evidence that the bones have fused. This often takes eight to 12 weeks.
Risks and complications
The majority of arthrodesis operations are uneventful and are not associated with complications, however, these are major procedures and thus the following complications are possible:
- loosening or breakage of implants (plates, screws, pins) may occur if the joint fails to fuse in sufficient time. Implant failure can result in joint instability and necessitate further surgery.
- wound problems, such as breakdown and infection, are primarily associated with arthrodesis of the carpal (wrist) and hock (ankle) joints. Wound management within the first few weeks of surgery is of vital importance to minimise this risk. Dressings are often applied to the limb to minimise swelling and prevent the patient interfering with the wound.
- fracture of bones adjacent to the fused joint may occur due to the abnormal forces that result following arthrodesis surgery.
How good is limb function following arthrodesis surgery?
Limb function after arthrodesis surgery is primarily dependent on which joint is fused. It is good following carpal (wrist) and hock (ankle) arthrodesis and fair following shoulder arthrodesis. Fusion of the elbow or stifle (knee) joint significantly compromises limb function. Dogs and cats generally have to swing the limb outwardly (circumduct) when walking in order to prevent the toes dragging on the ground.
Conclusion
In those patients where arthrodesis is indicated, the vast majority benefit from surgery. Fusion of a joint is undoubtedly a major undertaking, and these procedures are commonly performed by specialist orthopedic surgeons. We will be pleased to give as much help and support as possible if you decide to give your pet the opportunity of arthrodesis surgery.
Special Offer – May 2019
by admin on April 30th, 2019
Category: News, Tags:
Corneal Sequestrum
by admin on April 2nd, 2019
Category: News, Tags:
What is the cornea?
The cornea is the clear window of the eye. It is a very delicate structure which is less than a millimetre thick. In order to be transparent, the cornea has no blood vessels. This makes the cornea vulnerable to injury and infection, and results in a slow healing response to deep wounds.
What is a corneal sequestrum?
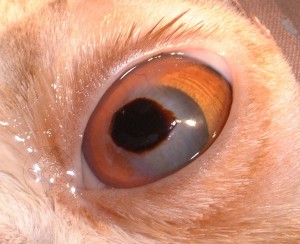
A corneal sequestrum is a part of the cornea which has died off and which is then rejected by the remaining healthy cornea. Most sequestra (as more than one sequestrum is known) affect the centre of the cornea. Corneal sequestra are usually pigmented in different shades of brown and may vary in appearance from subtle bronze staining to very obvious dark plaques. In some patients, blood vessels grow into the cornea in response to the sequestrum and a reddish rim may surround the pigmented plaque. In many affected patients, their tears will also be darkly pigmented and brown to black discharge may crust on the eyelids.
Is a corneal sequestrum a problem for affected cats?
Overall, the answer to this question is yes. In their very early stages, corneal sequestra will not cause pain or visual impairment but with time corneal ulceration (wounding) develops, and patients will show intermittent signs of eye pain such as blinking, squinting, weeping and light-shyness. Occasionally patients will show signs of a sequestrum only after several episodes of apparently spontaneous corneal ulceration.
Corneal sequestra can become infected, and this may lead to loss of the eye in the absence of rapid treatment.
What causes a corneal sequestrum?
Chronic injury has been identified as a possible cause of sequestrum formation and especially abnormalities of the eyelids such as inward turning of the eyelids and eyelashes. However, even today, it is not known why the majority of patients develop corneal sequestra. Many theories have been investigated and herpesvirus (one of the cat flu viruses) has been identified as a possible cause in crossbred (domestic short haired) cats. However, most corneal sequestra are seen in purebred cats such as Persians and British Short Hair cats. It is possible that the special shape of the faces of these patients is associated with the problem. They generally have big bulging eyes which often have a poor blinking response. Herpesvirus does not generally appear to be related to sequestrum developments in purebred cats. Abnormalities of the tear film such as a poor quality or quantity of tears are also considered to be involved in some cases.
What treatment options are available if my cat has a corneal sequestrum?
There are three major treatment options available:
- Conservative treatment with antibiotic and lubricating ointments to reduce irritation and prevent infection until the eye has shed the sequestrum by itself.
- Surgical excision of the sequestrum and placement of a soft contact bandage lens.
- Surgical excision of the sequestrum followed by a grafting procedure to provide support for the affected area of cornea and to reduce the risk of the sequestrum coming back.
In general, it is unlikely that continued conservative treatment will be recommended, as this is usually associated with prolonged periods of eye pain for the patient. Furthermore, ongoing monitoring and veterinary care will be required to try and reduce the risk of infection or rupture (bursting) of the cornea. This is a risk as the sequestrum may spread deeper. The cost advantage of not proceeding with surgery usually does not outweigh the prolonged care and discomfort for patients suffering a sequestrum, and the result of surgery may be less good with later intervention.
In our experience, surgical removal of the corneal sequestrum under the operating microscope is the treatment of choice. Given the depth of the lesion and the risk of retention of some pigment in the cornea after surgery, an additional grafting procedure may well be recommended.
Grafting procedures involve the placement of a piece of conjunctiva (the lining of the white of the eye) or other tissue into the wound following excision of the sequestrum. Grafts are usually stitched into place and will lead to a partial impairment of corneal transparency. However, the eye should still retain useful vision.
What does surgery for sequestrum removal involve?
Removal of corneal sequestra is carried out under general anaesthesia with the help of the operating microscope. The area around the eye is clipped. During the anaesthetic, the patient’s heart rate, blood pressure and blood oxygen concentration are monitored and a fluid infusion is given intravenously to maintain good blood circulation. Once the sequestrum has been removed, the surgeon will usually either place a contact lens or place a graft (see previously mentioned). Following the surgery, the operated eye is likely to be slightly sore and many cats will only partially open it for a few days.
What aftercare will be required?
Post-operatively, the patient needs to wear an Elizabethan collar to prevent damage to the wound by rubbing or scratching. Gentle cleaning of the operated eye with wet cotton wool twice daily is recommended.
An antibiotic ointment is generally applied to the eye for approximately ten days post-operatively. A short course of antibiotic tablets and painkillers may also be given after surgery. The use of false tears or other lubricant preparations may be recommended long-term in some cases, usually to be applied once or twice daily.
How successful is surgery for removal of a corneal sequestrum?
Surgical removal of corneal sequestra is a very successful surgery in uncomplicated cases.
The main risks of the procedure are wound infection and loosening of the graft. On occasion, a second procedure may be required to achieve a satisfactory result. Fortunately, the loss of an eye due to complications or progression of the disease after surgical sequestrum removal is very rare.
Surgery for sequestrum removal and placement of a graft aims at reducing the risk of sequestrum recurrence but cannot guarantee that the same eye will never be affected with another sequestrum.
Can my own veterinary surgeon remove the corneal sequestrum?
Removal of a corneal sequestrum is a procedure that requires a skilled and experienced micro-surgeon, equipment for magnification and illumination, and fine surgical instruments that will not damage the delicate tissues of the eye. For this reason most general practitioners will recommend referral to an ophthalmic specialist for treatment of this condition.
Do I have to return to the eye specialist for the aftercare?
After an eye has developed a serious disease which has required a major procedure, it is best to have its progress checked by the specialist. The number of revisits will depend upon the severity of the problem and the post-operative progress. In many cases only two or three re-visits will be required. In more complex cases there may be a need to continue with further check-ups from time to time.
Is my cat’s other eye at risk?
Unfortunately, the other eye is also at risk of sequestrum formation and must be carefully monitored for this reason. At the moment no treatment is known that will reliably prevent sequestrum formation, but the use of ocular lubricants may be helpful in providing some degree of additional corneal protection.
Cancer in cats and dogs: Surgical therapy
by admin on March 4th, 2019
Category: News, Tags:
The role of surgery in the management of the patient with cancer
Surgery is commonly used in the management of solid tumours (i.e. tumours that are ‘lumps’ rather than tumours such as leukaemia that are not just in one place) in dogs and cats.
Surgery may have a number of roles to play in the management of cancer:
- Surgery for diagnosis (biopsy)
- Surgery for prevention of cancer, i.e. removal of abnormal tissue before it becomes cancerous (e.g. pre-malignant change such as polyps), or removal of other tissue (e.g. testicles or ovaries) to prevent hormone-dependent cancer
- Definitive curative-intent
surgery, i.e. surgery designed to remove all of the tumour and cure the patient of that tumour - Cytoreductive surgery, i.e. surgery designed to remove most of the tumour and leave only microscopic deposits of tumour cells so that additional therapy (e.g. radiotherapy or chemotherapy) will be more effective
- Palliative surgery, i.e. surgery designed to improve the patient’s quality of life without necessarily extending the duration of life
The role of biopsy before surgical treatment
We need to understand what the role of surgery in any patient is before the operation is performed, so that it is as clear as possible what benefit the patient is likely to receive. This will generally require that a biopsy is obtained prior to other surgery, to identify the nature of the tumour. We will discuss these issues and the results of the biopsy with owners at each stage.
However, a biopsy may not be performed in the following circumstances, which are occasionally encountered:
- If the results of the biopsy would not change the plan for treatment, i.e. the treatment is the same regardless of the nature of the tumour
- If the results of the biopsy would not change the owner’s willingness to treat, i.e. if a particular treatment would be chosen, whatever the tumour is
- If the biopsy procedure is as invasive or difficult as surgical excision, i.e. to avoid two major surgical procedures
However, if we do not have information provided by a biopsy, we may be faced with an increased risk that the entire tumour is not subsequently removed and that a cure is not obtained.
Types of surgery
Curative-intent surgery
Curative-intent surgery (surgery designed to remove all of the tumour and cure the patient) represents the best option for many tumours, but it is only appropriate for a tumour or tumours in one location, with no evidence of spread. Surgery cures more patients of their tumour than any other treatment (e.g. radiotherapy, chemotherapy) and consideration is always given to surgery if it is possible.
The advantages of surgical management of cancer are:
- It provides an immediate cure (in appropriate circumstances)
- It does not cause cancer (as radiotherapy and chemotherapy might do)
- It has no toxic side effects
- It does not suppress the immune response
- It is effective for large masses, whereas radiotherapy or chemotherapy are not
Surgery may be combined with other types of treatment including chemotherapy and radiotherapy. Generally these additional therapies are used post-operatively, once the amount of tumour in the body has been reduced to as low a level as possible, to delay or prevent return or spread of the tumour. However, in some cases, these other treatments may be used before surgery to make the surgical procedure simpler or more likely to be successful.
When considering surgery for the management of cancer, the following principles should be borne in mind:
- A diagnosis should be established to help plan the surgical procedure
- Diagnostic imaging (X-rays, CT scan) should often be used to assess the extent of the tumour and improve our ability to plan the surgical procedure
- Surgery should be performed early in the course of the disease when the tumour is small, rather than allowing it to grow larger
- The first surgical procedure for any particular tumour has the best chance of success. If the tumour recurs after one surgery has been performed, it is difficult to know where the tumour now extends to
- Surgery for cure involves removing the tumour and a margin of normal tissue in 3 dimensions
It is important to realise that while curative intent surgery has a good chance of curing the patient of that tumour, the pet may develop additional new tumours in the future.
Cytoreductive surgery
Cytoreductive surgery involves the removal of all the tumour that can be seen with the naked eye, but accepts that microscopic deposits of tumour cells will be left behind and the patient will not be cured with surgery. However, reducing the number of tumour cells in the body increases the effectiveness of post-operative radiotherapy or chemotherapy, as these two types of treatment are less effective when dealing with a large mass.
This therapy will probably not produce a cure, but will often provide long-term local control, i.e. will prevent the mass from regrowing for as long as possible and will delay the signs of ill-health due to the tumour for as long as possible. Cytoreductive surgery generally involves a more minor procedure than surgery for cure and the recovery time after surgery is therefore generally shorter.
Palliative surgery
Palliative surgery is designed to remove a tumour that is causing signs of illness, while accepting, as for cytoreductive surgery, that this will not cure the patient. This surgery may be performed for tumours that are causing pain and discomfort or that are infected or ulcerated. Often this is a more effective form of pain relief than painkilling drugs alone. Usually, the simplest type of palliative surgery that will provide an improvement in the animal’s health is chosen, to maximise the benefit of this surgery, avoid a long recovery time and minimise post-operative complications.
Other considerations prior to surgery
For more radical surgery and, in particular, surgery that alters the appearance of the pet, e.g. surgery of the head and neck or amputation of a limb, pet owners understandably often have two concerns:
- How will surgery alter the cosmetic appearance of my pet?
- How will surgery affect the ability of my pet to lead a normal, happy life i.e. to function normally?
These questions are usually asked in that order. On reflection, we would probably all regard normal function to be more important than a normal appearance. However, the physical appearance of a pet is still an important factor in decision-making. This decision may sometimes be made easier if the pet is otherwise well and if radical surgery offers the potential for a cure, and if without therapy the tumour will likely lead to the pet being put to sleep.
Wound healing may be delayed or impaired in patients with cancer and a wound infection may be more common. This is as a result of the adverse effects that the tumour has on the body, and the effects of the therapy itself.
Surgical margins and types of surgery
If we are using surgery to attempt a cure, we will aim to remove the entire tumour along with a margin of normal tissue, to do all we can to ensure that all the tumour is removed. This margin of normal tissue is not exact and is our best guess at how far the tumour has invaded into the adjacent tissue.
Around the tumour, these margins are normally measured in centimetres, with more invasive tumours having wider margins (e.g. 3cm) than less invasive tumours (e.g. 1cm). Below the tumour, these margins are either measured in a similar way, or a natural barrier to tumour invasion is chosen, so that the tumour is removed with this barrier intact, as though removing the tumour in an “envelope” of normal tissue. A benign tumour may be removed with very narrow margins. In some locations, adequate margins of excision cannot be achieved while still preserving the function of the affected body part and a cure may not be achievable.
Cytoreductive surgery and palliative surgery procedures will generally remove the tumour with a narrow margin of tissue, as a cure is not anticipated.
Wound reconstruction
All surgical procedures for the management of cancer involve two steps:
- Removal of the tumour
- Reconstruction of the wound
Often, removal of the tumour is relatively straightforward, whereas reconstruction of the wound can take longer and be more of a challenge. The ability to close the wound in some way after surgery may dictate whether the tumour is considered operable. Normally several options are considered for closure of the wound in the planning stage, so that we have the best chance possible to provide a good outcome.
Post-operative pain management (analgesia)
We cannot discuss surgical management of cancer without discussing post-operative pain control (analgesia). Before embarking on any surgery we have to be sure that we can provide adequate analgesia for all our patients, irrespective of the underlying disease and the surgical procedure performed. It is also important to realise that for certain tumours, surgically removing the tumour is an effective means of providing pain relief, and as a result some patients are more comfortable in the immediate post-operative period than they were before surgery.
We aim to use analgesia drugs before there is any pain or discomfort (pre-emptive analgesia) in our patients and to use a combination of analgesic agents of different types that work in different ways and act at different sites in the body. As a result, our patients will often receive an aspirin-like drug (a non-steroidal anti-inflammatory drug: NSAID), a morphine-like drug (an opiate) and a local anaesthetic, as well as other types of drug.
Post-operative care
Patients will normally be kept in the hospital after surgery until the nursing care and analgesia that they need is relatively minor and can be provided by the owner at home. Instructions for post-operative care may comprise:
- Examination of the wound daily for any evidence of inflammation
- Administration of drugs, e.g. analgesia, antibiotics
- Exercise restriction until the surgical site has healed sufficiently
- Methods to prevent the patient licking or scratching at the surgical site.
Assessment of the tumour specimen and monitoring of the patient
Once the tumour is removed, it will normally be sent to the laboratory for assessment, even if a biopsy was obtained beforehand, as a larger sample can often provide additional information. Examination of the tumour specimen post-operatively may provide the following information:
- Confirmation of the type of tumour. In certain tumours, particularly those with various cell types in it, a small sample (such as that obtained at biopsy) may not be representative of the actual type of tumour
- Identification of the tumour grade, if this could not be assessed pre-operatively
- Evaluation of the local lymph nodes (glands) if these were not accessible before surgery, but could be sampled at surgery
- Assessment of the tumour margins as to whether all the tumour has been removed. This helps to predict the likelihood of tumour recurrence at the surgical site
- Identification of invasion of the blood vessels and lymph vessels by tumour cells. This helps to predict the likelihood of distant tumour spread elsewhere in the body
Our aim at every stage is to make sure that owners of pets undergoing surgical treatment for cancer are fully informed and understand what is being recommended and why. We will discuss possible complications and the likely costs involved ahead of time, and we will only undertake surgery with an owner’s fully informed consent and understanding.
Cancer in cats and dogs
by admin on February 1st, 2019
Category: News, Tags:
Assessment of the patient
Cancer is common in human and veterinary medicine. Approximately one quarter to one third of all our patients will suffer from cancer at some point in their lives, which is similar to the incidence of cancer in human medicine. So, we encounter a large number of patients with cancer during our clinical work, and we also find that many owners themselves will have some first-hand knowledge of cancer, which may affect the decisions they make about the disease in their pet.
The investigation and management of animals suspected of having cancer or known to have cancer is relatively straightforward and generally proceeds in a similar manner for all patients, with a few basic rules followed in a stepwise manner. When investigating a particular tumour, we never forget that the tumour is attached to a patient, and that we need to carefully consider the care and needs of the pet as well as those of their owner. Our approach is one of keeping owners fully informed at each step and making plans for investigation and management of the pet only after careful discussion with the owner.
Outline:
The following information is divided into the following sections:
- Investigation and care of the patient
- Investigation of the tumour
- Identification of the most appropriate therapy
The information is arranged in this way, because this is the way that our patients present to us and because we think of the patient first, his or her disease second and the proposed therapy third. In particular, we always make every effort to ensure that we have a correct diagnosis before we begin therapy and that the patient will be able to tolerate the treatment prior to us starting it.
1. Investigation of the patient
General assessment of the patient
When presented with an animal suspected of having or known to have cancer, our initial approach is to assess the patient and then assess the tumour. Each patient is different, as is each tumour, and the investigative approach is therefore tailored to the individual, although the same basic principles apply.
When presented with a patient with cancer, we want to get an accurate assessment of the long-term outlook or prognosis. The prognosis for animals with cancer depends on a number of factors:
- The microscopic or histological type of the tumour, i.e. what cells are in the tumour?
- The grade of the tumour, i.e. how aggressive do these cells look under the microscope?
- The clinical stage of the tumour, i.e. is there any evidence that the tumour is affecting more than one site in the body?
- The presence of tumour-related complications (so-called ‘paraneoplastic syndromes’)
- The presence of other diseases
Our approach is to:
- Assess the general health of the patient
- Identify any other diseases present
- Confirm the presence of a tumour
- Gain as much information as possible about the tumour
- Identify how the tumour is affecting the patient currently
The basic principles in assessing the patient with cancer comprise:
- Tumour measurement
- Staging the tumour
- Assessment of the patient’s general health and fitness
- Diagnostic imaging (e.g. X-rays, ultrasound, CT scan, MRI scan)
- Blood samples to look at the various blood cells and other substances in the blood (haematology and biochemistry)
- Examination of samples from the tumour or other sites, either samples of cells (cytology) or tissue (histology)
Two important factors are the grade and stage of the tumour, both of which must be assessed. Grade is assessed under the microscope and compares the tumour cells to the normal cells of the same type.
- Grade predicts the biological behaviour of the tumour, e.g. benign or malignant and how different from normal the cells look
- Grade answers the question ‘How might the tumour affect the patient in the future?’
Stage is assessed clinically and with diagnostic imaging and sometimes samples of cells or tissues.
- Stage tells us where the tumour is within the patient, e.g. is it restricted to the site where it started growing, or has it spread to other tissues, e.g. lymph glands (lymph nodes) and other organs
- Stage answers the question ‘How is the tumour affecting the patient right now?’
Tumour staging
One of the most important ways to assess the patient with cancer, is the ‘TNM’ system. This involves:
- Examination of the primary Tumour (with a biopsy – see later)
- Assessment of the regional lymph Nodes (the ‘glands’ such as we have in our necks)
- Assessment of other sites for Metastasis (spread elsewhere)
Staging is generally performed by a combination of physical examination, diagnostic imaging and taking biopsy samples of the tumour to look at under the microscope (‘cytology’ or ‘histology’). In some cases, the appearance on diagnostic imaging may be sufficient to make a diagnosis without biopsy, e.g. nodules in the lungs seen on an X-ray of the chest suggests spread of cancer cells to the lungs.
This clinical staging represents the ‘gold standard’. However, this approach is not necessary or appropriate in all cases. For instance, for a pet with a benign tumour confirmed with a biopsy taken by sucking cells out of the tumour through a hypodermic needle (needle biopsy), the prognosis (outlook) is excellent and the likelihood of tumour spread is very low, so staging may be taken no further after gaining some information about the primary tumour.
Care of animals with cancer
We all may have our own view of how the tumour is affecting the pet and owners may well have other concerns about their pets apart from the fact that they have a tumour. The supportive care of the patient is the second part of compassionate patient care, after ‘diagnosis’ and before ‘therapy’. This is important, since we wish to avoid the tendency to leap from diagnosis to treatment without considering what supportive care is needed.
Our approach can be summarised by three important rules, which we all consider:
- We should ensure that our patients do not experience pain or discomfort associated with the tumour or its treatment
- We should ensure that our patients are able to eat a normal amount of food to meet their nutritional requirements, and if they cannot, we should think about how to help them to do so
- We should ensure that our patients do not suffer side effects of the tumour or therapy, such as vomiting or feeling sick when undergoing treatment, if at all possible
Management of chronic cancer pain
When asked what our concerns about cancer would be, most of us would say that pain associated with cancer would be uppermost in our minds. As a rule, we understand how to manage acute pain after an operation (see later), but the management of chronic cancer pain in a patient where a total cure is not possible is sometimes more difficult to achieve.
We have detailed methods of assessment of pain and discomfort and understand the importance of treating and managing any pain or discomfort associated with cancer. It is important to realise that management of pain does not just involve drugs traditionally thought of as ‘painkillers’ but may also include other drugs that have an effect on the way nerves and the brain deal with pain (e.g. gabapentin and amitryptiline) or drugs and other therapies that have an effect on the tumour itself (e.g. bisphosphonates or radiotherapy in cases of the bone tumour, osteosarcoma).
We should also bear in mind that in some tumours the most successful method of pain relief may be surgical removal of the tumour itself, whether that is a procedure designed to cure the patient or a treatment designed to remove or reduce the clinical signs associated with the presence of the tumour without totally curing it.
2. Investigation of the tumour
Tumour biology
As a general rule, if we do not understand the basic biology of a disease i.e. the behaviour of the cancer cells in the patient’s body, we cannot provide appropriate treatment. One important lesson that has emerged from both human and veterinary oncology over the past few years is that, when it comes to cancer, the biology of the disease will dictate what happens in the long-term.
A common question asked when a diagnosis of cancer is made in our pet is ‘What caused the cancer?’ While we know something about some causes of cancer (and what is happening in the cancer cells and their genes), for the most part, we do not know the cause.
The total number of cells in a person or animal is a balance between the number of cells growing and those dying. For a long time it has been considered that cancer is a disease caused by uncontrolled cell growth. However, of more importance is the fact that cancer cells refuse to die when programmed to do so (this programmed, and perfectly normal, cell death is called ‘apoptosis’). Cancer therapies that encourage cell death are likely to be just as important as, if not more important, than therapies that prevent cell growth.
Other examples of cutting edge treatments in humans that have been developed as a result of understanding tumour cell biology include those designed to stop the early phase of tumour spread (metastasis) by preventing tumour cells moving through the tissue, and those causing a reduction in tumour growth by preventing the tumour causing the growth of new blood vessels (angiogenesis) which the tumour needs in order to grow.
Tumour pathology
Pathologists play a critical role in the investigation of the patient with cancer by examining tissue from the primary tumour (the original site of the growth) and, in some cases, the lymph nodes and other potential sites for spread (metastasis).
Assessment of cells obtained from a mass with a hypodermic needle (cytology) is often the first approach in the diagnosis of an animal suspected of having cancer, but in most animals, examination of a tissue sample (histology) is necessary at some point during the assessment of the patient.
Histological assessment of the tumour may also provide more specific information regarding the outlook or prognosis:
- Examination of the tumour edges after the growth has been surgically removed may tell us whether the tumour is likely to grow back in the same place (i.e. if there are tumour cells at the edge of the specimen, it is likely that tumour cells have been left in the patient)
- Examination of a large specimen for evidence of tumour cells spreading into the blood vessels or lymph drainage vessels may suggest whether the tumour is likely to spread
Other effects of the tumour (Paraneoplastic syndromes)
Paraneoplastic syndromes are additional effects that cancer might have in parts of the body away from the primary (or original) tumour. These abnormalities may have an effect on the patient’s health and may affect their ability to tolerate sedation or anaesthesia and treatment. The paraneoplastic syndrome may be the main reason for the animal being taken to the veterinary surgeon in the first place (the owner may not even realise that there is a tumour somewhere) and these syndromes also may provide a useful guide to the success of therapy, i.e. if the paraneoplastic syndrome gets better, this suggests that the tumour tissue has been removed or destroyed. In rare cases, the paraneoplastic syndrome may be very obvious but the location of the underlying primary tumour is more difficult to find, even for the veterinary surgeon. In such cases, additional imaging procedures can prove very helpful.
Examples of these syndromes are alterations in the number of red blood cells or white blood cells in the circulation and abnormalities in the blood level of glucose or certain salts or ‘electrolytes’ (e.g. calcium).
3. Treatment of the patient with cancer
Achieving a diagnosis
As a general rule, a biopsy (taking cells or a larger piece of the tumour for analysis) is needed before beginning any therapy, unless we have a good reason not to take a biopsy. A biopsy may be omitted if knowing more about the tumour would not change the treatment plan or the willingness to treat the patient. However, care is taken to ensure that these reasons apply in any individual patient. A biopsy should always be tailored to the individual tumour and we will always consider whether a biopsy of the regional lymph node (gland) or other sites of potential metastasis (spread) is needed at the same time.
Selecting the best cancer treatment for the patient
Once a diagnosis has been achieved and we have information on clinical staging, the effect of the tumour on the patient and any concurrent diseases, and once we have identified whether the patient needs additional supportive care, we can start to consider different treatment options.
The main treatment options for the management of cancer are:
- Surgery: The physical removal of the tumour
- Radiotherapy: The use of a strong X-ray beam to destroy the cancer cells where they sit
- Chemotherapy: The use of anti-cancer drugs to kill cancer cells wherever they are
Each of these has specific advantages and disadvantages and may be used singly or in combination. All of the factors listed above, particularly the tumour type, grade, stage and location and the presence of other health problems will help to decide what the most appropriate therapy is. Therapy may be designed to cure the patient or to remove the signs of illness for as long as possible, if a complete cure is not possible.
In addition, other ways of treating various types of cancer are becoming more common in human oncology, and these benefits will become available for our patients in due course.
These include:
- Immunotherapy, e.g. vaccination with melanoma-specific antigens in patients with melanoma (a tumour of the pigment cells in the body)
- Targeted therapy with small molecule inhibitors, e.g. tyrosine kinase inhibitors (TKIs) which may be used in some patients with mast cell tumours
Monitoring the response to therapy
Once the cancer has been treated, the patient will still be monitored in various ways, depending on the nature of the tumour and the aim of the therapy. This may involve a number of the tests (e.g. blood samples, X-rays) used to make the diagnosis in the first place and a plan for monitoring will be tailored to the needs of the patient. This may include:
- Monitoring for the return (local recurrence) of the tumour at the original site
- Examining for the presence of tumour spread elsewhere
- Monitoring for the development of new primary tumours at other sites
If you have any questions about your pet’s condition, or his or her treatment, please do not hesitate to contact us.